Inflammatory bowel disease (IBD) affects over 2 million Americans. While advances in medical therapy have improved the care of IBD patients, many still suffer from refractory disease with significant morbidity. IBD includes two distinct clinical phenotypes called Crohn’s disease and ulcerative colitis. Although genetic polymorphisms correlate with disease susceptibility, environmental triggers including diet and intestinal bacteria are thought to play a central role in disease pathogenesis. While certain intestinal bacteria may act as opportunistic pathogens causing infection and inflammation, we and others have shown that microbiota function as a double-edged sword by simultaneously working to maintain homeostasis at mucosal surfaces. Thus, the major focus of our work is to define the cellular, molecular, and microbial regulation of intestinal barrier immunity and to develop novel diagnostic and therapeutic approaches for medically refractory IBD.
Post-doctoral fellowship positions available!
Please email Randy at ral2006@med.cornell.edu
Immunology and Mucosal Healing in IBD
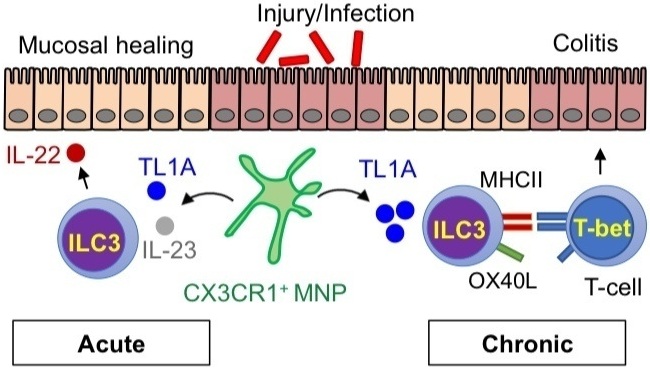
One part of our lab focuses on understanding the cellular and molecular mechanisms of homeostatic inhibition/induction by microbes within the intestine. Questions remain regarding the bacterial signals impacting immune cells in the intestine, the local and molecular signals regulating these interactions, and the in vivo role in mucosal healing.
The Microbiome of Extra-intestinal Manifestations
A second part of the lab focuses on microbial changes associated with extra-intestinal manifestations (EIMs) of IBD and their influence on mucosal and systemic immunity. By studying patients with IBD-associated SpA, we have a unique opportunity to understand the process by which luminal microbes shape systemic immune repertoires.
Click here to read more about our work on IBD and joint inflammation>
Translational Research at the Jill Roberts Center
We are committed to performing high-quality research with direct implications for improving the diagnostics and therapeutics in the treatment of IBD. This includes specific studies on the role for fecal microbiota transplantation in ulcerative colitis, medical therapy and the microbiome in Crohn's disease associated joint inflammation, and the role for new emerging therapy.